Overview
The public Telehealth Services Analysis available at civhc.org provides important information about the utilization of telehealth services and payments made for telehealth services in Colorado. The analysis includes all public and private health insurance payers submitting data to the Colorado All Payer Claims Database (CO APCD), which represents the majority of covered lives (70% of medically insured) in the state. This analysis includes claims data for the following calendar years: 2019 through 2023.
This analysis tracks telehealth based largely on Governor Jared Polis’ expanded definition in Colorado statute (C.R.S. § 10-16-123(4)(e)(I)).
The intent of this analysis is to provide information related to the use of telehealth services across the state prior to, during, and after the onset of the COVID-19 pandemic.
This analysis helps answer several key questions about telehealth services pre- and post-onset of COVID-19:
- How has telehealth use changed as a result of the pandemic?
- Have the types of telehealth services patients are accessing changed?
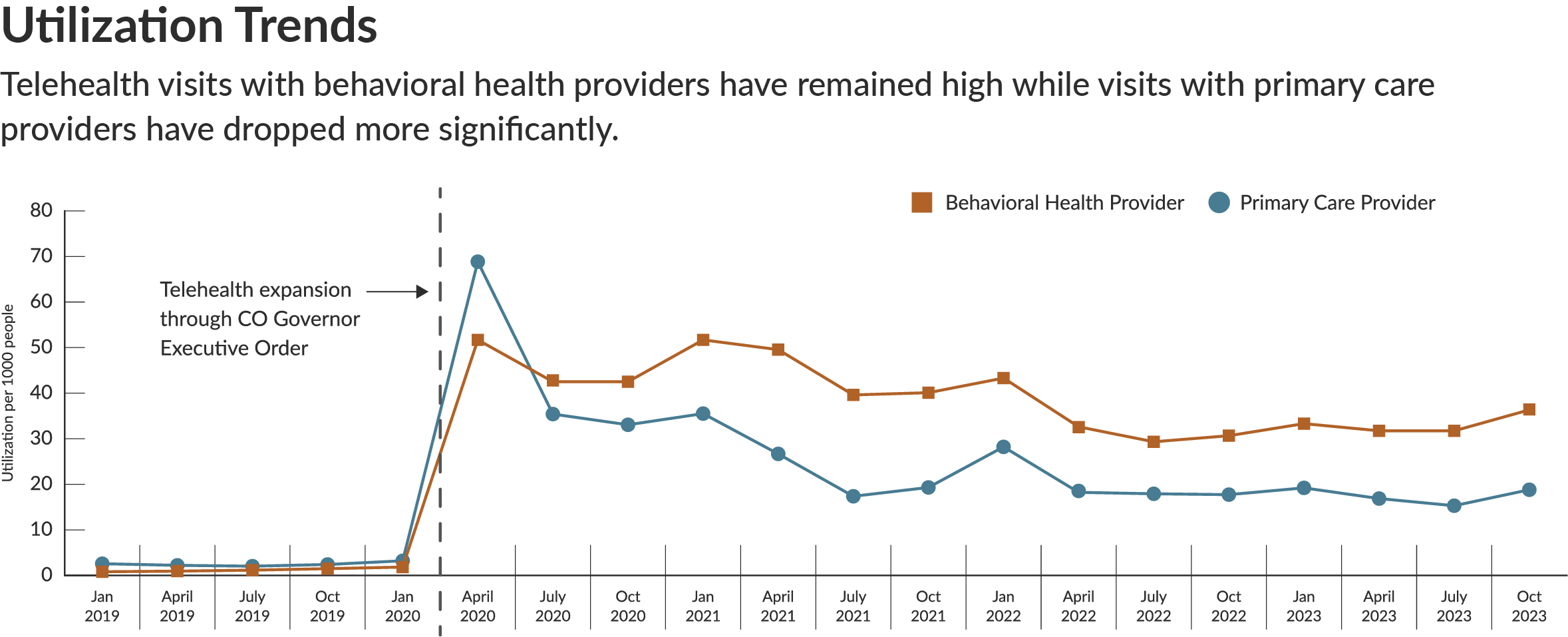
- Are different providers now delivering telehealth services?
- How does the of use telehealth differ between counties across the state?
- How much are we spending on telehealth per person and as a state?
- What are the top behavioral health conditions being treated via telehealth?
- What are the trends in telehealth use post-pandemic?
- Who are the primary users of telehealth?
- This analysis includes the majority of insured lives in Colorado, but does not include all self-insured employer covered lives, or federal health insurance programs such as the Veterans Administration, Tricare, and Indian Health Services.
- When viewing the data by provider type, Federally Qualified Health Center and Rural Health Clinic information is lower than expected because the analysis only captures visits when they are billed under their facility taxonomy and does not capture providers billing under a different taxonomy code (i.e. primary care).
- This analysis includes visits paid for through fee-for-service only, and do not include any supplemental payments or visits/payments that occurred through Alternative Payment Models.
-
Use Cases
Utilize insights to shape telehealth regulations, assess policy impacts on telehealth use, and target areas to increase equitable telehealth access.
Study shifts in telehealth utilization and its effects on health care delivery and cost-efficiency, providing evidence for future health care studies and policy recommendations.
Understand how telehealth use differs across communities in the state, and work with state agencies and providers to expand access in underserved areas.